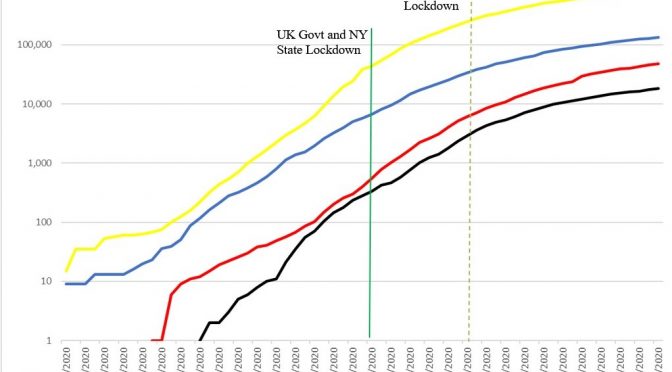
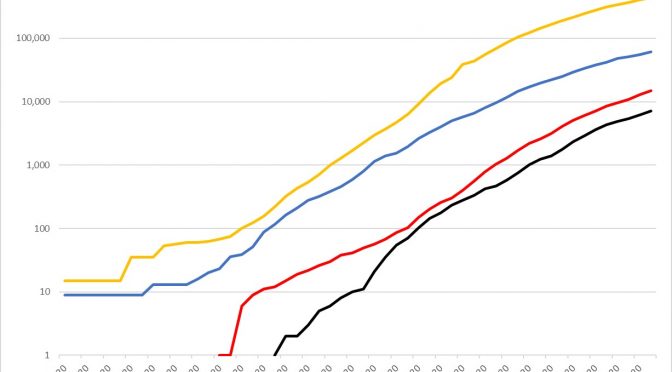
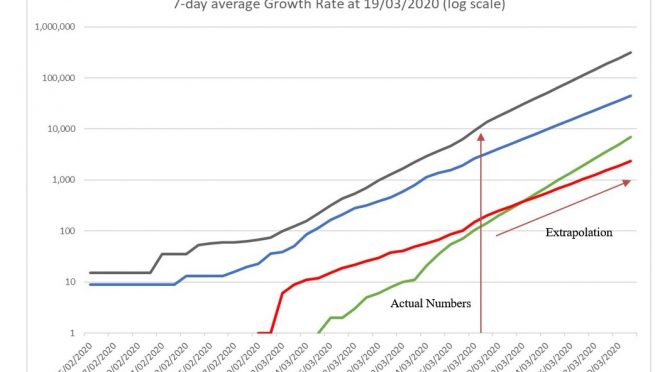
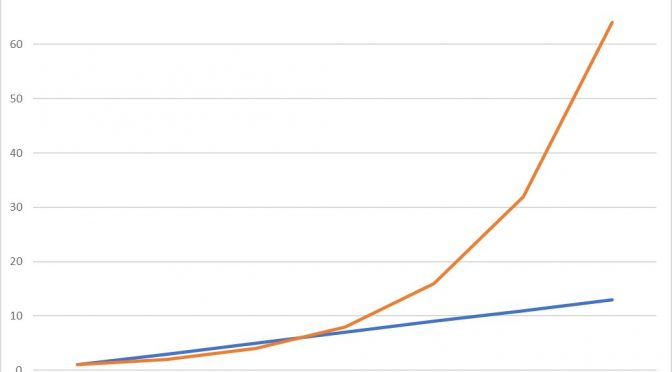
As anticipated, the Coronavirus outbreak has definitively entered new phases in both the UK and the US, in the wake of ‘lockdown’ restrictions limiting non-essential production and consumption and encouraging populations to stay at home. These policies are centralised in the UK and State-wide in most of the US. As we can see from Chart […]